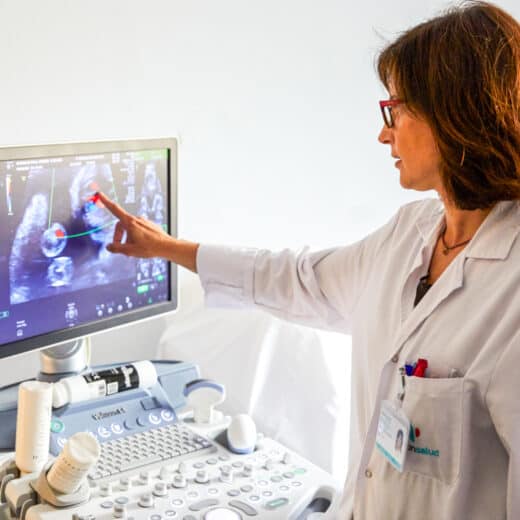
Medical Careers
Why Practice Rural Medicine?
About Kasey
Kasey Isaacs is a senior at Morehead State University and is pursuing his Bachelor's degree in Biomedical Sciences, with an emphasis in Pre-Medicine. A recipient of the Atlantis Pre-med Leaders Scholarship, he spent three weeks on an Atlantis Clinical Shadowing Fellowship in Milan, Italy in Summer 2017.
With more and more doctors choosing to work in metropolitan hospitals, it is important to understand the potential benefits of practicing medicine in a rural setting. Today, Kasey walks us through his decision to pursue rural medicine.
Remembering My Roots
As an aspiring doctor, it can be difficult to look past the coursework, MCAT prep, shadowing and stress of the pre-med years. All are important concerns, but we must not let them cloud the realities of the career we have chosen to pursue. One such reality is the healthcare crisis facing rural America.
Modern medical practice, for all its advancements, has been unable to solve this far-reaching problem. As a resident of Appalachia, this is particularly concerning to me. In the article below, I aim to elucidate the situation for those of you who are unfamiliar with it and inspire you to consider pursuing a career in rural medicine, so that together we can begin to alleviate this burden.
The Need
Rural American populations face significant health disparities when compared to urban populations. The National Rural Health Association (NHRA) found that several factors work in tandem to create such conditions. These include lower access to physicians, higher incidence of disease and disability, longer distance to the nearest healthcare facility, lower average household income, and higher levels of tobacco use.
Many of the nation’s leading killers—including heart disease, cancer, and stroke—depend heavily on the fast action that many rural Americans simply are unable or unwilling to choose.
What Is “Rural”?
In order to address the problem, we need a clear understanding of the terms. What exactly does “rural” mean?
Providing a quantifiable definition is no easy task. According to Webster’s Dictionary, rural is an adjective that means “of or relating to the country, country people or life, or agriculture.” Though succinct and accurate, this doesn’t provide much information in terms of actual demographic parameters.
The U.S. Census Bureau defines a rural area to be any territory, housing, or population that is not urban—a classification that is, of course, meaningless without a definition of urban. Currently, “urbanized areas” have a population of 50,000 people or more, while “urban clusters” contain between 2,500 and 50,000 people.
Considering this data, we can conclude that roughly 20 percent of the American population resides in rural areas. This may appear to be a paltry statistic at first glance, but the total sum is nearly 60 million people.
The Primary Care Shortage
The healthcare disparity that exists in rural regions is particularly evident in terms of primary care providers. According to the National Center for Health Statistics, the patient-to-primary care physician ratio in rural areas is only 39.8 physicians per 100,000 people, compared to 53.3 physicians per 100,000 in urban areas.
But how does this tangibly affect the health of people in this region?
Consider the geographical distance that exists between 100,000 people in rural areas, as opposed to the same number in urban centers. Rural Americans must travel greater distances to reach healthcare providers, which in turn means they must take more time off work and foot the bill for the fuel required, all the while making an average salary of roughly $9,000 less than comparable urbanites.
Such financial concerns can lead to the dismissal of potentially life-threatening diseases, as it is too complicated or expensive to seek medical attention. Then, because of delay, this can lead to more severe presentations. Many of the nation’s leading killers—including heart disease, cancer, and stroke—depend heavily on the fast action that many rural Americans simply are unable or unwilling to choose.
The very existence of government agencies like the Federal Office of Rural Health Policy prove that we have not been idle in attacking this crisis. Now, as aspiring physicians, we have access to innumerable university-sponsored programs aimed at tackling these issues.
Fixing the Problem
Now that I have presented the problem, you may wonder: what is being done to combat it?
The very existence of government agencies like the Federal Office of Rural Health Policy (FORHP) as well as the many research groups they fund, including the North Carolina Rural Health Research and Policy Analysis Center (NC RHRP), and the Rural and Underserved Health Research Center prove that we have not been idle in attacking this crisis. The group’s data collection and other initiatives have amplified awareness of this issue, and medical educational institutions have responded in kind.
As aspiring physicians, we now have access to innumerable university-sponsored programs aimed at tackling these issues. These university-sponsored programs are tailored to those interested in rural medicine – particularly primary care – and include the following:
The Kenan Primary Care Medical Scholars Program – UNC School of Medicine
The Rural Physician Leadership Program – University of Kentucky College of Medicine
ROME Rural Scholars Program – Texas College of Osteopathic Medicine
Rural Physician Program – Michigan State University College of Human Medicine
Rural Medical Scholars Program – University of Alabama School of Medicine
Trover Rural Track – University of Louisville School of Medicine
Thankfully, the programs listed above are only a sampling of what United States academic institutions have to offer.
Financial Incentives to Pursue Rural Medicine
Although the dire need for improved healthcare in rural regions has inspired many a doctor, there are also financial incentives that make rural medicine a worthwhile pursuit for students. Financially speaking, the decision to practice rural medicine makes medical school much more affordable. Through the National Health Service Corps, students may even be able to earn a full medical school scholarship.
The Health Resource and Service Administration (HRSA)—a branch of the U.S. Department of Health and Human Services—uses a variety of criteria to determine areas of the United States that are either Health Professional Shortage Areas (HPSAs) or Medically Underserved Areas/Populations (MUA/Ps). As one may expect, a large amount of the areas designated as HPSAs or MUA/Ps are located in rural regions throughout the nation.
An HRSA subdivision known as the National Health Service Corps (NHSC) offers varying amounts of loan repayment for health professionals that will agree to work at NHSC-approved sites—sites that are determined to be in need based directly on their HPSA score.
Licensed healthcare professionals that commit to working at an NHSC-approved site for two years can earn up to $50,000 toward their student loans, with the full $50,000 being allotted to those working in sites with the highest HPSA score.
Furthermore, medical (or dental) students in their final year of school can earn $120,000 toward their student loans if they agree to work in an NHSC site of greatest need for three years through the Student to Service Program.
[READ ALSO]: The Reality of Medical School Debt
As an additional source of loan forgiveness, the NHSC site also provides information on State Loan Repayment Programs. These are cost-sharing federal grants provided to certain—largely rural—states that have a high number of HPSAs. Such programs are aimed at primary care providers in particular and are designed to allow healthcare institutions to attract the healthcare professionals that they need to begin alleviating the burden of local shortages. Actual commitment years, exact financial details, and the disciplines that are eligible vary from state to state.
However, the financial relief is not limited to loan repayment only.
For those committed to fulfilling the role of a primary care physician provider early in their professional career, the NHSC offers the ultimate prize: a full ride to medical school.
This is no joke.
NHSC scholarship recipients are provided with a living stipend in addition to fully paid tuition, fees, and educational costs. In return, students simply agree to work at an approved NHSC site for the same amount of years that they receive aid (which is capped at four years).
Summarily, agreeing to work as a primary care provider in an NHSC site for four years allows you to leave medical school with zero debt—easily a $250,000+ value.
Rural Lifestyle Benefits
If the pride of addressing a national health crisis and the delight of saving money is not incentive enough, I have one final alluring proposal. The lifestyle offered in rural America—in my very biased opinion—is second to none.
Cultural emphasis on such ideals as faith, family, independence, and hard work combine with breathtaking mountains, beautiful farmland, and innumerable lakes, valleys, streams, and woodlands to create opportunities for both lifestyle decisions and leisure that simply cannot be had elsewhere.
The list of recreational activities available in rural America is nearly unending and should be particularly attractive to those who love outdoor adventure. In my own small county alone, popular pastimes include boating, fishing, hiking, wakeboarding, skiing, swimming, spelunking, rock climbing, hunting (particularly deer and turkey), kayaking, off-roading, target shooting, archery, and horseback-riding.
Add to these the opportunity to live in peaceful, secluded vales, expansive farms, or simply neighborhoods with multiple acre yards and the draw of rural living becomes a bit more apparent.
And did I mention the views?
I realize the rural life is not for everyone. However, if you love serenity and the great outdoors, you ought to consider it.
I hope I’ve Presented a Convincing Case.
In summary, here are the reasons you should at least consider a career in rural medicine.
First and foremost, the need is there. Rural Americans suffer from subpar healthcare access. As the rising generation of healthcare professionals, we must strive to address this. Medical schools have recognized the need and are beginning to train physicians specifically for practice in rural regions. Additionally, the government has established programs and allocated funds to address this disturbing trend.
As current students and future practitioners, we have the tools necessary to begin fixing this healthcare disparity. It is now up to us, particularly we who have a love and passion for rural America and the lifestyle it provides, to seize the opportunity and turn this problem around.
Our Alumni Enter Great Medical Schools

John Daines
- Atlantis '17
- Brigham Young University '19
- Washington U. in St. Louis MD '23


Zoey Petitt
- Atlantis '17
- U. of Arizona '18
- Duke MD '23

Zoey Petitt
Hungary ’17 || University of Arizona (undergraduate) ’18
Completed Atlantis Program Location and Date:
Hungary, Summer 2017
Do you believe your Atlantis experience helped you get into your graduate program?
I believe it was very helpful.
Generally, why do you think Atlantis helped you get into your graduate program?
For me, my Atlantis experience played a key role in confirming my decision to go into medicine. This was important for me to discuss during the admissions process.
Specifically, did you talk about Atlantis in your interviews?
Yes

Yong-hun Kim
- Atlantis '17
- Stanford '19
- Mayo Clinic MD '24

Yong-Hun Kim
Budapest, Hungary ’17 || Stanford University
Program:
Budapest, Hungary – Winter 2017
Undergraduate:
Stanford University class of 2019
Major:
Computer Science
Honors:
Bio-X Grant (award for research)
Undergraduate Activities:
President and Founder of Stanford Undergraduate Hospice and Palliative Care, Volunteer for Pacific Free Clinic, Research Assistant in Wernig Pathology Lab, President of Hong Kong Student Association, violin performance
Describe Atlantis in three words:
Eye-opening. Spontaneous. Exhilarating.
Why did you choose Atlantis?
I chose the Atlantis program because it combines opportunities to shadow physicians and travel abroad, both of which I had little prior exposure to.
What was your favorite experience as an Atlantis participant?
My favorite experience as an Atlantis participant came in the stories exchanged over meals or excursions and the breadth of conversation that reflected the diversity of backgrounds within our cohort and site managers.
What was the most meaningful aspect of your time shadowing?
I appreciated the chance to speak with physicians in Budapest and hear their personal motivations for pursuing medicine because it really helped better contextualize and validate my own interest in medicine. The physicians were also just really welcoming, relatable, and down-to-earth people.
How has Atlantis helped equip you for the future?
The Atlantis program has equipped me with a better understanding of what a career in medicine looks like, which I think is an invaluable gift considering the long road ahead of those who aspire to be a physician.
How has Atlantis equipped you for active leadership in the medical field?
The ability to interact and empathize with patients of diverse backgrounds and communities is a necessity to be a leader in the medical field. I think the Atlantis program, through my interactions with mentors and their patients, has helped me take my first steps toward attaining the cultural vocabulary and literacy required of a physician.

Megan Branson
- Atlantis '18
- U. of Montana '19
- U. of Washington MD '24


Sarah Emerick
- Atlantis '19
- Eckerd College '20
- Indiana U. MD '25

Snow Nwankwo
- Atlantis '19
- Catholic U. of America '21
- Georgetown U. MD '26


Tiffany Hu
- Atlantis '16
- U. of Maryland '17
- U. of Michigan MD '22

Tiffany Hu
Tereul, Spain ’16 || U Michigan Medical School
Program:
Teruel, Spain – Summer 2016
Undergraduate:
University of Maryland class of 2017
Admitted medical student at:
University of Michigan Medical School
Major:
Neurobiology
Honors:
Honors Integrated Life Sciences Program, Banneker/Key Scholarship
Extracurricular Activities:
American Medical Student Association Co-President & Advocacy Day Liaison, Alternative Breaks Experience Leader, Health Professions Advising Office Student Advisory Board, Biology Teach Assistant, Health Leads, Buddhist Tzu Chi Foundation, NIH Research Intern, Physicians for Social Responsibility Environment & Health Intern
Describe Atlantis in Three Words:
Educational. Eye-opening. Exhilarating.
Why did you choose Atlantis?
I wanted to expand my horizons and understand a culture of health different from the ones I am accustomed to. I had shadowed doctors in the United States and Taiwan prior to my Atlantis program experience, and being able to see first-hand the healthcare system in Spain allowed me to draw comparisons between the different complex healthcare systems.
What was your favorite experience as an Atlantis participant?
Bonding with the other participants and celebrating our time together along with the doctors we shadowed. We would discuss our interests, passions, and motivation for medicine, and it was an incredible experience to learn from and alongside them.
What was your experience with the doctors you were shadowing?
Because of the pre-established relationships with the hospitals in which we shadowed, all the doctors were very welcoming and accommodating. They were willing to translate for us and explain in detail all of their medical decisions. My doctors and I had wonderful conversations about the differences between life in Spain vs. the United States.
What was the most meaningful aspect of your time shadowing?
I was excited to scrub in on surgeries and watch as the doctor explained what he was doing throughout the operation. Before and after surgeries, as well as in my other rotations, I observed how the doctors reassured and communicated with their patients. I was able to glean insight into differences between the experience of health in Spain versus the United States through observation as well as conversations with the doctors.
How has Atlantis helped equip you for the future?
Besides the wealth of medical knowledge I gained from shadowing the doctors, I challenged myself to step outside of my cultural comfort zone and explore more than I thought I was capable of. Atlantis allowed me to make connections with people from all around the United States and abroad, and the friendships I gained helped me learn so much more than I would have on my own.

Lauren Cox
- Atlantis '18
- Louisiana Tech '20
- U. of Arkansas MD '24

Lauren Cox
Libson, Portugal ’18 || Louisiana Tech
Completed Atlantis Program Location(s):
Lisbon, Portugal
Year of most recent program:
Fall ’17 – Summer ’18
Season of most recent program:
Summer
Do you believe your Atlantis experience helped you get into your graduate program?
Extremely helpful
Generally, why do you think Atlantis helped you get into your graduate program?
It exposed me to shadowing that was hard to come by in the states. It also gave me a chance to see other systems of healthcare.
Specifically, did you talk about Atlantis in your interviews? If so, how much relative to other topics?
Yes – they wanted to know about my experience, and specifically how the healthcare I saw in another country compared to what I had seen in the USA.

Kayla Riegler
- Atlantis '18
- U. of Kentucky '20
- U. of Kentucky MD '24

About Atlantis
Atlantis is the leader in pre-health shadowing and clinical experience, offering short-term programs (1-10 weeks) over academic breaks for U.S. pre-health undergraduates. Medical schools want 3 things: (1)healthcare exposure, (2)GPA/MCAT, and (3)certain competencies. Atlantis gives you a great version of (1), frees you to focus on (2), and cultivates/shows (3) to medical school admissions committees.

Watch Video: The Atlantis Shadowing Experience and How it Helps In Your Med/PA Admissions Future

Two Atlantis alumni admitted to Top 5 MD programs wrote our widely read medical school admissions guidebook — download yours.
Get our 76-page medical school admissions guidebook, by Atlantis alumni at Harvard Medical School and Stanford School of Medicine.