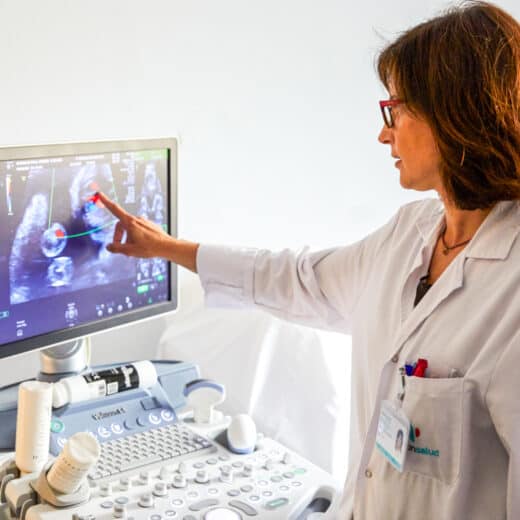
Applying to Med/PA School, Medical Careers
NP, PA or MD? Deciphering Your Healthcare Career Choices
About The Atlantis Team
We offer helpful, informative content to the next generation of healthcare professionals, so that they can achieve their goals, avoid common pitfalls, and grow in their passion for healthcare.
Public Opinions about Medical Careers
You arrive at a social function and begin to make your rounds, shaking hands and sharing small talk. As you get to know new acquaintances, their inevitable questions arise: What are you studying? What do you want to do after college?
It’s a familiar scenario. If your experiences have been anything like mine, articulating your dream of becoming a physician can lead to a flurry of questions and opinions. I’ve received comments ranging from “You should be a Nurse Practitioner — that’s where the future is” to “Good for you! We need more real doctors around here.”
All students with medical aspirations owe it to themselves and their future patients to find their proper niche, where they can utilize their greatest strengths for the benefit of the greatest number.
At the same time, the large assortment of healthcare career paths, acronyms, and job duties can get overwhelming.
To tackle all such paths in one article would be impossible (or at least unreadable), so instead let’s look at one of the most common points of confusion. What are the differences between Nurse Practitioners, Physicians Assistants, and Physicians (both MD and DO)?
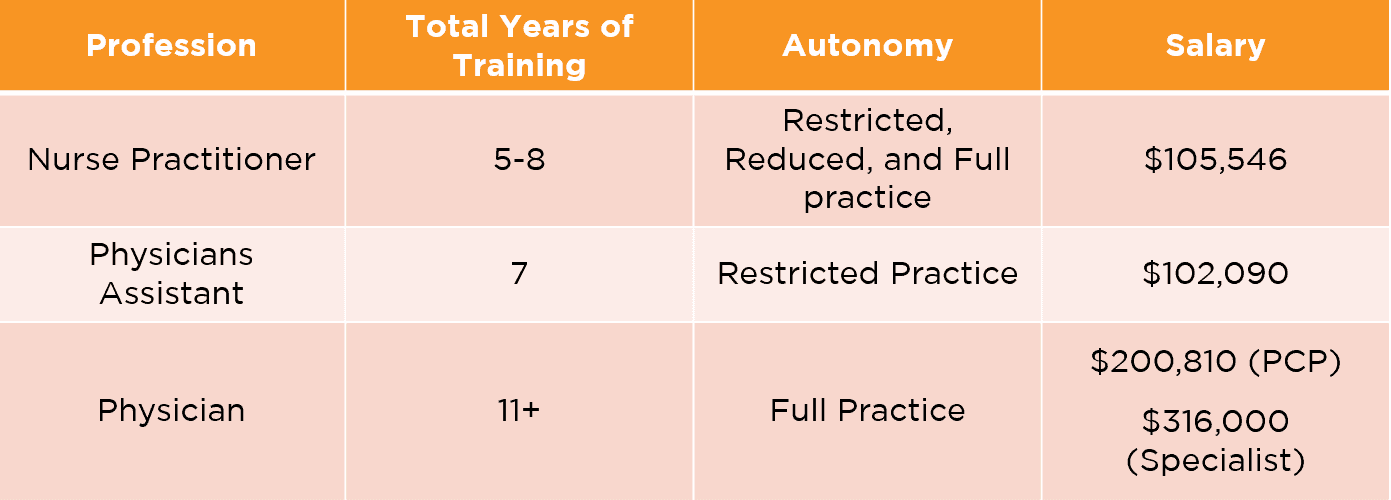
Before we begin, it’s important to note that all of the professions I listed above may serve as primary care providers; you can find them writing prescriptions, consulting patients, and otherwise appearing to perform the same tasks and duties. However, this can result in misconceptions. So let’s take a closer look and dissect the differences in role, training, autonomy, and salary.
The chart below highlights the total amount of time spent in training, the amount of autonomy allowed in the day-to-day of the job, and the expected salary of each profession.
Nurse Practitioners (NPs)
How to Become a Nurse Practitioner
According to the American Association of Nurse Practitioners (AANP), NPs are “clinicians that blend clinical expertise in diagnosing and treating health conditions with an added emphasis on disease prevention and health management.” Though the requirements for certification differ between states and the type of healthcare setting, all begin their education by obtaining a nursing undergraduate degree (BSN), which involves passing the NCLEX-RN exam and becoming a registered nurse (RN).
Registered nurses can then attend either a Master of Science in Nursing (MSN) or a Doctor of Nursing Practice (DNP) program, which generally takes around three years to complete. Many Nurse Practitioners do not directly enter graduate school after undergrad, but instead opt to work as a BSN in order to gain clinical experience, which some graduate programs (but not all) require.
Job Autonomy of a Nurse Practitioner
The autonomy of NPs within their specialty of choice differs by state and tends to be a hot topic for debate within the world of healthcare. Currently, the laws are varied and can be a bit confusing. Though all NPs may prescribe medications, the types of medications (narcotics in particular) differ per local laws. Additionally, some states (known as restrictive) only allow NPs to practice under the supervision of a physician. In other states, NPs are allowed full autonomy, while others have arrangements that fall somewhere in the middle.
“The autonomy of NPs within their specialty of choice differs by state and tends to be a hot topic for debate within the world of healthcare.”
NPs are also specialized, choosing one or more specialties from a set of patient population focus areas. However, the vast majority of NPs (86.6%) are certified in an area of primary care, indicating that this is their primary role within the United States.
Salary of Nurse Practitioners
As far as salary goes, NPs are well paid for their work, averaging $105,546 per year in 2017. The average registered nurse who does not continue on to become a nurse practitioner can expect to make an average salary of $68,450 per year.
Physician Assistants (PAs)
The Physician Assistant is another common mid-level provider. PAs share some marked similarities with NPs, but they differ in many ways as well.
The main role of a PA is to perform examinations, diagnose patients, prescribe treatment plans, provide medical consultation, and otherwise perform many of the same tasks as physicians, while under a physician’s supervision.
According to the American Academy of Physician Assistants, “PAs are certified as medical generalists with a foundation in primary care.” The main role of a PA is to perform examinations, diagnose patients, prescribe treatment plans, provide medical consultation, and otherwise perform many of the same tasks as physicians, while under a physician’s supervision.
How to Become a Physician Assistant
PAs are usually not nurses. Those on the PA track do not attend a nursing undergraduate program, but instead may pursue a variety of majors. In fact, PA programs are more similar to medical school programs in that they require a set of prerequisite courses, including anatomy, physiology, microbiology, general biology, and chemistry. Thus, you will find many pre-PAs majoring in subjects like biology and chemistry.
The hallmark of most PA programs is their clinical hour requirement. Prior to admittance into PA school, students are encouraged to obtain around three years of hands-on experience in a role such as paramedic, technician, or Certified Nursing Assistant (CNA).
Thus, those who attend an undergraduate program as a traditional student must find the time to work hundreds, if not thousands, of clinical hours should they wish to apply directly to a PA program, while simultaneously fulfilling the needs of a demanding major.
The curricula of PA programs are derived from those of medical schools, and it takes about three years to complete the program (including a year of supervised rotations). Once a PA has graduated and passed the relevant national certification exam, he or she is free to practice under the supervision of a physician.
Job Autonomy of a Physician Assistant
Whereas NPs can sometimes practice without the supervision of a consulting physician, Physician Assistants generally work under the guidance of an MD or DO. As with NPs, the states have varying laws regarding the limitations of practice and prescriptions that can be handled by PAs.
In 2016 data found by the Statistical Profile of Certified Physicians Assistants, only 27.8% of PAs were found to work in primary care. The remaining percentage worked within a variety of specialties and subspecialties (including cardiology, gastroenterology, etc.), and surgical specialties.
Salary of a Physician Assistant
PAs are compensated on a similar level as NPs, with a mean 2016 salary of $102,090. While they may be operating in a way that more resembles a physician, their salary tends to be lower because the number of hours worked is usually lower and more regular than those of an MD or DO. PAs can generally decide to work a routine schedule during the week.

“The hallmark of most PA programs is their clinical hour requirement. Prior to admittance into PA school, students are encouraged to obtain around three years of hands-on experience in a role such as paramedic, technician, or Certified Nursing Assistant (CNA).”
Physicians (MDs and DOs)
Physicians are the most intensively trained clinicians, benefiting from a rigorous curriculum designed to produce highly skilled and compassionate healthcare leaders. They are responsible for maintaining the physical and mental health of the populace through the utilization of medically informed diagnoses, evidence-based treatments, cutting-edge technology, patient education, and considerate care. They exist in all manner of specialties and subspecialties across the full spectrum of healthcare.
Prospective medical students must complete the required prerequisites for medical school, which usually include biology, general and organic chemistry, basic physics, English and school-specific recommended or required courses. Many pre-med students major in biology, one of its various biomedical offshoots, chemistry, or the like.
Physicians are the most intensively trained clinicians, benefiting from a rigorous curriculum designed to produce highly skilled and compassionate healthcare leaders.
How to Become a Physician
By junior year, pre-meds take the Medical College Admission Test (MCAT) and apply to medical school. Once accepted, they receive two years of extensive training in advanced courses pertinent to their career (anatomy, pharmacology, human behavior, etc.) and then go on to two years of rotations throughout the many different specialties of medicine.
Job Autonomy of a Physician
After completing their fourth year, medical students become physicians and move on to residency, where they further hone and refine their skills for a minimum of three years before being able to practice on their own. In sum, this entails a minimum of 11 years of training. However, once they are fully trained, they are entirely autonomous in their particular practice. This means that they are directly observing symptoms, weighing the options, choosing a method of treatment, and ordering the execution of the treatment without needing to consult an authority figure. This does not mean that doctors don’t consult with other physicians, nurses, residents, etc., but they are able to act entirely on their own.
Salary of a Physician
The compensation for this intensive track is proportional to the time and effort it demands. In 2017, primary care physicians earned an average salary of $200,810 per year. Specialists, who undergo even more training, averaged a healthy $316,000. This may seem like a huge jump in salary, but it is important to remember how much extra time and money goes into the training necessary to become a specialized physician. Considering the average debt of a newly trained physician, these salaries are often times necessary to pay back their student debt.
Conclusion
As you hopefully have seen in the paragraphs above, physicians and other clinicians share many similarities, but also a number of differences.
No matter the part you play, an effective healthcare system takes a full team of professionals to run efficiently. Although every member is vital, physicians act as the leaders. Contrary to what some may think, this does not imply an elevation of status, but rather a willingness to serve and bear the burden of intense education, long hours, frustrating systems, mountains of paperwork, and great responsibility.
“Ultimately, whether you aspire to be an NP, PA, MD or DO, remember this: whichever healthcare path you choose, your priority must always be to provide the highest level of patient care.”
In recent years, however, NPs and PAs have taken on more autonomy and responsibility as many doctors have moved toward specialties and hospital employment. The trend is multifaceted and may be attributed to a series of interconnected issues including rising medical school tuition (prompting students to seek a higher paying specialty), the primary care provider (PCP) shortage, changes in healthcare culture, faster tracks to practice for PAs and NPs, and of course political influence.
Ultimately, whether you aspire to be an NP, PA, MD or DO, remember this: whichever healthcare path you choose, your priority must always be to provide the highest level of patient care. In what other world do the decisions so often literally mean life or death?
Our Alumni Enter Great Medical Schools

John Daines
- Atlantis '17
- Brigham Young University '19
- Washington U. in St. Louis MD '23


Zoey Petitt
- Atlantis '17
- U. of Arizona '18
- Duke MD '23

Zoey Petitt
Hungary ’17 || University of Arizona (undergraduate) ’18
Completed Atlantis Program Location and Date:
Hungary, Summer 2017
Do you believe your Atlantis experience helped you get into your graduate program?
I believe it was very helpful.
Generally, why do you think Atlantis helped you get into your graduate program?
For me, my Atlantis experience played a key role in confirming my decision to go into medicine. This was important for me to discuss during the admissions process.
Specifically, did you talk about Atlantis in your interviews?
Yes

Yong-hun Kim
- Atlantis '17
- Stanford '19
- Mayo Clinic MD '24

Yong-Hun Kim
Budapest, Hungary ’17 || Stanford University
Program:
Budapest, Hungary – Winter 2017
Undergraduate:
Stanford University class of 2019
Major:
Computer Science
Honors:
Bio-X Grant (award for research)
Undergraduate Activities:
President and Founder of Stanford Undergraduate Hospice and Palliative Care, Volunteer for Pacific Free Clinic, Research Assistant in Wernig Pathology Lab, President of Hong Kong Student Association, violin performance
Describe Atlantis in three words:
Eye-opening. Spontaneous. Exhilarating.
Why did you choose Atlantis?
I chose the Atlantis program because it combines opportunities to shadow physicians and travel abroad, both of which I had little prior exposure to.
What was your favorite experience as an Atlantis participant?
My favorite experience as an Atlantis participant came in the stories exchanged over meals or excursions and the breadth of conversation that reflected the diversity of backgrounds within our cohort and site managers.
What was the most meaningful aspect of your time shadowing?
I appreciated the chance to speak with physicians in Budapest and hear their personal motivations for pursuing medicine because it really helped better contextualize and validate my own interest in medicine. The physicians were also just really welcoming, relatable, and down-to-earth people.
How has Atlantis helped equip you for the future?
The Atlantis program has equipped me with a better understanding of what a career in medicine looks like, which I think is an invaluable gift considering the long road ahead of those who aspire to be a physician.
How has Atlantis equipped you for active leadership in the medical field?
The ability to interact and empathize with patients of diverse backgrounds and communities is a necessity to be a leader in the medical field. I think the Atlantis program, through my interactions with mentors and their patients, has helped me take my first steps toward attaining the cultural vocabulary and literacy required of a physician.

Megan Branson
- Atlantis '18
- U. of Montana '19
- U. of Washington MD '24


Sarah Emerick
- Atlantis '19
- Eckerd College '20
- Indiana U. MD '25

Snow Nwankwo
- Atlantis '19
- Catholic U. of America '21
- Georgetown U. MD '26


Tiffany Hu
- Atlantis '16
- U. of Maryland '17
- U. of Michigan MD '22

Tiffany Hu
Tereul, Spain ’16 || U Michigan Medical School
Program:
Teruel, Spain – Summer 2016
Undergraduate:
University of Maryland class of 2017
Admitted medical student at:
University of Michigan Medical School
Major:
Neurobiology
Honors:
Honors Integrated Life Sciences Program, Banneker/Key Scholarship
Extracurricular Activities:
American Medical Student Association Co-President & Advocacy Day Liaison, Alternative Breaks Experience Leader, Health Professions Advising Office Student Advisory Board, Biology Teach Assistant, Health Leads, Buddhist Tzu Chi Foundation, NIH Research Intern, Physicians for Social Responsibility Environment & Health Intern
Describe Atlantis in Three Words:
Educational. Eye-opening. Exhilarating.
Why did you choose Atlantis?
I wanted to expand my horizons and understand a culture of health different from the ones I am accustomed to. I had shadowed doctors in the United States and Taiwan prior to my Atlantis program experience, and being able to see first-hand the healthcare system in Spain allowed me to draw comparisons between the different complex healthcare systems.
What was your favorite experience as an Atlantis participant?
Bonding with the other participants and celebrating our time together along with the doctors we shadowed. We would discuss our interests, passions, and motivation for medicine, and it was an incredible experience to learn from and alongside them.
What was your experience with the doctors you were shadowing?
Because of the pre-established relationships with the hospitals in which we shadowed, all the doctors were very welcoming and accommodating. They were willing to translate for us and explain in detail all of their medical decisions. My doctors and I had wonderful conversations about the differences between life in Spain vs. the United States.
What was the most meaningful aspect of your time shadowing?
I was excited to scrub in on surgeries and watch as the doctor explained what he was doing throughout the operation. Before and after surgeries, as well as in my other rotations, I observed how the doctors reassured and communicated with their patients. I was able to glean insight into differences between the experience of health in Spain versus the United States through observation as well as conversations with the doctors.
How has Atlantis helped equip you for the future?
Besides the wealth of medical knowledge I gained from shadowing the doctors, I challenged myself to step outside of my cultural comfort zone and explore more than I thought I was capable of. Atlantis allowed me to make connections with people from all around the United States and abroad, and the friendships I gained helped me learn so much more than I would have on my own.

Lauren Cox
- Atlantis '18
- Louisiana Tech '20
- U. of Arkansas MD '24

Lauren Cox
Libson, Portugal ’18 || Louisiana Tech
Completed Atlantis Program Location(s):
Lisbon, Portugal
Year of most recent program:
Fall ’17 – Summer ’18
Season of most recent program:
Summer
Do you believe your Atlantis experience helped you get into your graduate program?
Extremely helpful
Generally, why do you think Atlantis helped you get into your graduate program?
It exposed me to shadowing that was hard to come by in the states. It also gave me a chance to see other systems of healthcare.
Specifically, did you talk about Atlantis in your interviews? If so, how much relative to other topics?
Yes – they wanted to know about my experience, and specifically how the healthcare I saw in another country compared to what I had seen in the USA.

Kayla Riegler
- Atlantis '18
- U. of Kentucky '20
- U. of Kentucky MD '24

About Atlantis
Atlantis is the leader in pre-health shadowing and clinical experience, offering short-term programs (1-10 weeks) over academic breaks for U.S. pre-health undergraduates. Medical schools want 3 things: (1)healthcare exposure, (2)GPA/MCAT, and (3)certain competencies. Atlantis gives you a great version of (1), frees you to focus on (2), and cultivates/shows (3) to medical school admissions committees.

Watch Video: The Atlantis Shadowing Experience and How it Helps In Your Med/PA Admissions Future

Two Atlantis alumni admitted to Top 5 MD programs wrote our widely read medical school admissions guidebook — download yours.
Get our 76-page medical school admissions guidebook, by Atlantis alumni at Harvard Medical School and Stanford School of Medicine.