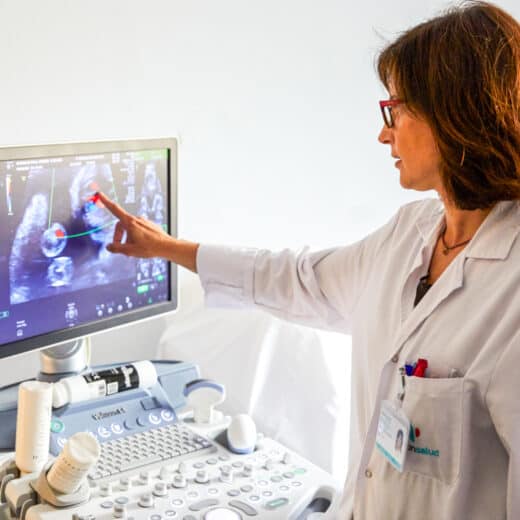
Applying to Med/PA School
How to Prepare for MMI Interviews
About The Atlantis Team
We offer helpful, informative content to the next generation of healthcare professionals, so that they can achieve their goals, avoid common pitfalls, and grow in their passion for healthcare.
MMIs, or Multiple Mini Interviews, are becoming a popular method of interviewing medical school applicants. They are unpredictable, and therefore daunting, but we have some tips for you to handle them with confidence.
Interview Day:
Your heartbeat thuds in your ears, as your blood pumps wildly through your veins. It’s not life or death, but it sure feels that way. You turn around and there’s the prompt in stark black letters on the whiteboard. After shaking clammy hands with your interviewer, you sit down. The Multiple Mini-Interview (MMI) has begun.
Created in 2002 by McMasters University, MMIs generally consist of a series of brief interviews in a timed circuit. In the past decade, medical schools have increasingly employed MMIs in lieu of one or two traditional long interviews, so it’s important to familiarize yourself with the format.
But what prompted the switch in the first place? According to the Association of American Medical Colleges, MMIs “[produce] a more reliable assessment of a candidate and limits interview biases due to the number of interactions.” Whereas a few long interviews are much higher stakes and a slip-up will have greater impact, MMIs aren’t make-it-or-break-it precisely because there are so many mini-interviews (usually between 6 and 12).The theory behind the MMI is that multiple smaller interviews will allow interviewers to better understand your values, thought patterns, and other soft skills such as the ability to empathize and problem-solve.
Between a Rock and a Hard Place
MMIs are often centered around a specific ethical dilemma or scenario. Although that might sound intimidating, it’s also a benefit for you because there are no right answers. However, while there may be no right answers, there are better or worse ways to answer an MMI prompt.
In this article, I’m going to give some tips on how to approach MMI interviews, with an emphasis on ethical problems. I won’t give any solutions, but I will equip you with the right questions to ask yourself. These questions should act as a framework that will guide your thoughts towards crafting a robust and thoughtful answer to any prompt you’re given. Remember, it’s more about your approach than your answer.
Here’s a general tip to start: Relax. Look, I’ve tried to cram philosophy papers the night before they’re due; but, frankly, that approach never turns out well. Some situations require a calm, slow thought process; philosophy and MMIs are some of those instances. If you’re frantic, you won’t be able to form coherent thoughts. Take a deep breath — the goal is not to convince your interviewers of your particular viewpoint, or even to fix the problem at hand. Your goal is to show your values and how you approach problems. Remember, as Dr. Jessica Friedman, a former medical admissions committee member at Mt. Sinai School of Medicine, says: there’s no wrong answer to an MMI prompt.
These questions should act as a framework that will guide your thoughts towards crafting a robust and thoughtful answer to any prompt you’re given.
Medical Ethics and the MMI
To start, let’s examine an important bioethical problem (and personal interest of mine) that often shows up in MMI questions: resource-allocation in times of scarcity. Often, we have a shortage of resources and a preponderance of need. Unfortunately, this means that not all those who need help will receive it. But how do we choose who does?
Organ transplantation is a classic example. Let’s say you’re a transplant surgeon, and you have one available liver. You alone get to decide who will receive it. (Note: this is not a plausible scenario, but an interesting one to ponder nonetheless.)
You have two patients in front of you: a 50-year-old man (Patient X) whose liver has degraded due to alcoholism. There are no complications; if he receives the liver, he will almost certainly recover and his system will regain full functioning capacity.
Next to him is another 50-year-old man (Patient Y): a father of three whose liver is riddled with cancer. His daughter is about to graduate from high school and is planning on attending university next year. Patient Y will definitely improve with a liver transplant, but there’s no guarantee he’ll be cancer-free.
To whom do you give the liver? On the one hand, we have a man who will certainly recover, but may have “deserved” his illness in the first place. On the other, we have a man who did nothing to merit his disease, but has uncertain chances for recovery.
The Four Principles of Medical Ethics
The best way to appraise a medical dilemma is to analyze it using the four principles of medical ethics. These principles were developed by Dr. Tom Beauchamp and Dr. James Childress and were published in their book Principles of Biomedical Ethics (1985). As America’s first significant bioethics text, this book soon became a standard reference, and its approach to medical ethics is widely accepted today.
Beauchamp and Childress’s methodology emphasizes approaching each situation with regard to four medical principles, now often called the “Four Pillars of Medical Ethics.” These include (1) autonomy, (2) beneficence, (3) non-maleficence, and (4) justice. They are defined as the following:
- autonomy: the patient controls the right to body and future
- beneficence: the doctor seeks to do good
- non-maleficence: the doctor avoids doing bad
- justice: the doctor treats all patience equally
Let’s start with Principle 1. In this case, both patients have successfully maintained their autonomy. Each has requested an organ, and it now falls upon you, the doctor, to attempt to provide it. You are not forcing the organ on either patient, nor are you ignoring the patients’ wishes. Thus, this situation does not violate principles of autonomy.
Next, let’s talk about Principle 4. This organ allocation dilemma is an ongoing medical debate that hinges upon the concept of justice. Many ask the question: Isn’t it unjust to give a liver to a patient who self-inflicted his own suffering when it could be given to a patient whose illness was tragically random?
In my opinion, that is not a fair question for a doctor to consider. As medical professionals, we serve justice. But be careful not to conflate justice with revenge. It is not up to the physician to mete out punishment; you are neither the judge, nor the jury, and especially not the executioner. Our duty is not to make sure people “get what they deserve”; it is to ensure all are treated justly, i.e. with equity.
Of course, your opinion may differ from mine. If you disagree, be prepared to justify why your motivations are not vindictive, and how they actually serve a greater good. One such way to approach this is to argue that an alcoholic is more likely to continue abusing alcohol and damage his liver all over again; thus, a cancer patient would be more deserving. In this way, giving the liver to a cancer patient would maximize the liver’s utility. Regardless of whether you agree, let’s examine the other facets of this dilemma.
Regardless of which option you choose, make sure you have examined the situation in regards to all four principles and be ready to demonstrate how each relates to your decision.
The remaining principles—beneficence and non-maleficence—often go hand-in-hand. Here, doing good can be seen as providing the liver to the person with the greatest potential for a full recovery. In this case, Patient X is most likely to make a full recovery, provided he stops drinking. Because Patient Y may suffer a relapse, his chances are lower. From this perspective, I can do more good and less bad by giving the liver to Patient X.
Thus, after putting all emotion and bias aside, it seems to me that the doctor ought to give the liver to Patient X, the alcoholic. My argument hinges on Principles 2 and 3 (Beneficence and Non-Maleficence), and posits that Principles 1 (Autonomy) and 4 (Justice) are less relevant.
If you disagree, you’re likely to cite Principle 4 as the basis of your argument. Regardless of which option you choose, make sure you have examined the situation in regards to all four principles and be ready to demonstrate how each relates to your decision.
Summary
This is only one example of how you should approach a bioethical dilemma.
To re-cap:
- Summarize the issue in all its ethically relevant facets
- Analyze the situation in respect to each of the four Principles of Medical Ethics
- State the conclusion, mentioning which principles justify your decision
Armed with this methodology, you won’t be so nervous when you face an MMI and questions about medical ethics problems. Remember, as long as you’re consistent in your principles and keep patient welfare foremost in mind, there are no wrong answers. Take a breath, speak with confidence, and go impress your interviewers!
Our Alumni Enter Great Medical Schools

John Daines
- Atlantis '17
- Brigham Young University '19
- Washington U. in St. Louis MD '23


Zoey Petitt
- Atlantis '17
- U. of Arizona '18
- Duke MD '23

Zoey Petitt
Hungary ’17 || University of Arizona (undergraduate) ’18
Completed Atlantis Program Location and Date:
Hungary, Summer 2017
Do you believe your Atlantis experience helped you get into your graduate program?
I believe it was very helpful.
Generally, why do you think Atlantis helped you get into your graduate program?
For me, my Atlantis experience played a key role in confirming my decision to go into medicine. This was important for me to discuss during the admissions process.
Specifically, did you talk about Atlantis in your interviews?
Yes

Yong-hun Kim
- Atlantis '17
- Stanford '19
- Mayo Clinic MD '24

Yong-Hun Kim
Budapest, Hungary ’17 || Stanford University
Program:
Budapest, Hungary – Winter 2017
Undergraduate:
Stanford University class of 2019
Major:
Computer Science
Honors:
Bio-X Grant (award for research)
Undergraduate Activities:
President and Founder of Stanford Undergraduate Hospice and Palliative Care, Volunteer for Pacific Free Clinic, Research Assistant in Wernig Pathology Lab, President of Hong Kong Student Association, violin performance
Describe Atlantis in three words:
Eye-opening. Spontaneous. Exhilarating.
Why did you choose Atlantis?
I chose the Atlantis program because it combines opportunities to shadow physicians and travel abroad, both of which I had little prior exposure to.
What was your favorite experience as an Atlantis participant?
My favorite experience as an Atlantis participant came in the stories exchanged over meals or excursions and the breadth of conversation that reflected the diversity of backgrounds within our cohort and site managers.
What was the most meaningful aspect of your time shadowing?
I appreciated the chance to speak with physicians in Budapest and hear their personal motivations for pursuing medicine because it really helped better contextualize and validate my own interest in medicine. The physicians were also just really welcoming, relatable, and down-to-earth people.
How has Atlantis helped equip you for the future?
The Atlantis program has equipped me with a better understanding of what a career in medicine looks like, which I think is an invaluable gift considering the long road ahead of those who aspire to be a physician.
How has Atlantis equipped you for active leadership in the medical field?
The ability to interact and empathize with patients of diverse backgrounds and communities is a necessity to be a leader in the medical field. I think the Atlantis program, through my interactions with mentors and their patients, has helped me take my first steps toward attaining the cultural vocabulary and literacy required of a physician.

Megan Branson
- Atlantis '18
- U. of Montana '19
- U. of Washington MD '24


Sarah Emerick
- Atlantis '19
- Eckerd College '20
- Indiana U. MD '25

Snow Nwankwo
- Atlantis '19
- Catholic U. of America '21
- Georgetown U. MD '26


Tiffany Hu
- Atlantis '16
- U. of Maryland '17
- U. of Michigan MD '22

Tiffany Hu
Tereul, Spain ’16 || U Michigan Medical School
Program:
Teruel, Spain – Summer 2016
Undergraduate:
University of Maryland class of 2017
Admitted medical student at:
University of Michigan Medical School
Major:
Neurobiology
Honors:
Honors Integrated Life Sciences Program, Banneker/Key Scholarship
Extracurricular Activities:
American Medical Student Association Co-President & Advocacy Day Liaison, Alternative Breaks Experience Leader, Health Professions Advising Office Student Advisory Board, Biology Teach Assistant, Health Leads, Buddhist Tzu Chi Foundation, NIH Research Intern, Physicians for Social Responsibility Environment & Health Intern
Describe Atlantis in Three Words:
Educational. Eye-opening. Exhilarating.
Why did you choose Atlantis?
I wanted to expand my horizons and understand a culture of health different from the ones I am accustomed to. I had shadowed doctors in the United States and Taiwan prior to my Atlantis program experience, and being able to see first-hand the healthcare system in Spain allowed me to draw comparisons between the different complex healthcare systems.
What was your favorite experience as an Atlantis participant?
Bonding with the other participants and celebrating our time together along with the doctors we shadowed. We would discuss our interests, passions, and motivation for medicine, and it was an incredible experience to learn from and alongside them.
What was your experience with the doctors you were shadowing?
Because of the pre-established relationships with the hospitals in which we shadowed, all the doctors were very welcoming and accommodating. They were willing to translate for us and explain in detail all of their medical decisions. My doctors and I had wonderful conversations about the differences between life in Spain vs. the United States.
What was the most meaningful aspect of your time shadowing?
I was excited to scrub in on surgeries and watch as the doctor explained what he was doing throughout the operation. Before and after surgeries, as well as in my other rotations, I observed how the doctors reassured and communicated with their patients. I was able to glean insight into differences between the experience of health in Spain versus the United States through observation as well as conversations with the doctors.
How has Atlantis helped equip you for the future?
Besides the wealth of medical knowledge I gained from shadowing the doctors, I challenged myself to step outside of my cultural comfort zone and explore more than I thought I was capable of. Atlantis allowed me to make connections with people from all around the United States and abroad, and the friendships I gained helped me learn so much more than I would have on my own.

Lauren Cox
- Atlantis '18
- Louisiana Tech '20
- U. of Arkansas MD '24

Lauren Cox
Libson, Portugal ’18 || Louisiana Tech
Completed Atlantis Program Location(s):
Lisbon, Portugal
Year of most recent program:
Fall ’17 – Summer ’18
Season of most recent program:
Summer
Do you believe your Atlantis experience helped you get into your graduate program?
Extremely helpful
Generally, why do you think Atlantis helped you get into your graduate program?
It exposed me to shadowing that was hard to come by in the states. It also gave me a chance to see other systems of healthcare.
Specifically, did you talk about Atlantis in your interviews? If so, how much relative to other topics?
Yes – they wanted to know about my experience, and specifically how the healthcare I saw in another country compared to what I had seen in the USA.

Kayla Riegler
- Atlantis '18
- U. of Kentucky '20
- U. of Kentucky MD '24

About Atlantis
Atlantis is the leader in pre-health shadowing and clinical experience, offering short-term programs (1-10 weeks) over academic breaks for U.S. pre-health undergraduates. Medical schools want 3 things: (1)healthcare exposure, (2)GPA/MCAT, and (3)certain competencies. Atlantis gives you a great version of (1), frees you to focus on (2), and cultivates/shows (3) to medical school admissions committees.

Watch Video: The Atlantis Shadowing Experience and How it Helps In Your Med/PA Admissions Future

Two Atlantis alumni admitted to Top 5 MD programs wrote our widely read medical school admissions guidebook — download yours.
Get our 76-page medical school admissions guidebook, by Atlantis alumni at Harvard Medical School and Stanford School of Medicine.